Contagion in our midst
by Stanley Perlman, MD, PhD
Human beings have been infected with viruses probably since we first evolved as a species. But as viruses are extremely small, it is only in the last 50 to 100 years that they were even characterised to a significant extent. However, the relationship between humans and viruses has changed over the past few years and some viruses that previously infected only wild or domesticated animals have now jumped the species barrier to infect humans (zoonotic viruses).
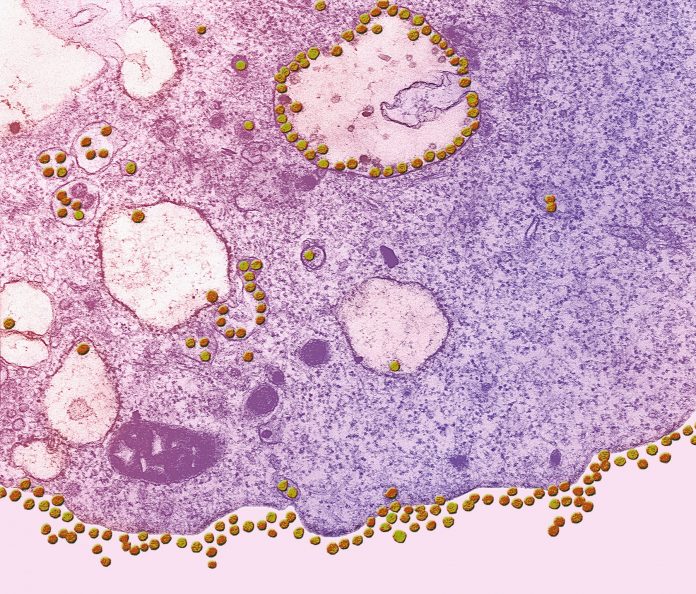
This occurred partly because humans have invaded the habitats of different animals. In addition, healthcare providers have become better at diagnosing these virus infections. Two of the most striking examples of this species jumping are the Severe Acute Respiratory Syndrome CoV (SARS-CoV) and the Middle East Respiratory Syndrome CoV (MERS-CoV). Both of these coronaviruses originated in bats, where they cause mild or subclinical infections. Both then infected an intermediate host, which probably served as the source for human infection.
SARS-CoV spread from bats to infect animals such as Himalayan civets and raccoon dogs in wet markets in China, and subsequently to human populations. It took a confluence of (unlucky) events for SARS-CoV to become as severe a human infection as it did and to spread to places all around the world.
SARS-like CoV probably crossed into human infections many times in the Chinese wet markets, but widespread transmission required infection of a highly susceptible individual, who spread the virus to others. Molecular epidemiological studies showed that the virus was rapidly adapting to the human host during the 2002–2003 epidemic before it was controlled.
In contrast, MERS-CoV spread from camels and perhaps other animals to humans. MERS-CoV causes upper respiratory tract infections in camels and has been in camel populations for at least 20 years. The MERS outbreak has been confined to countries in the Arabian Peninsula and travellers from that part of the world.
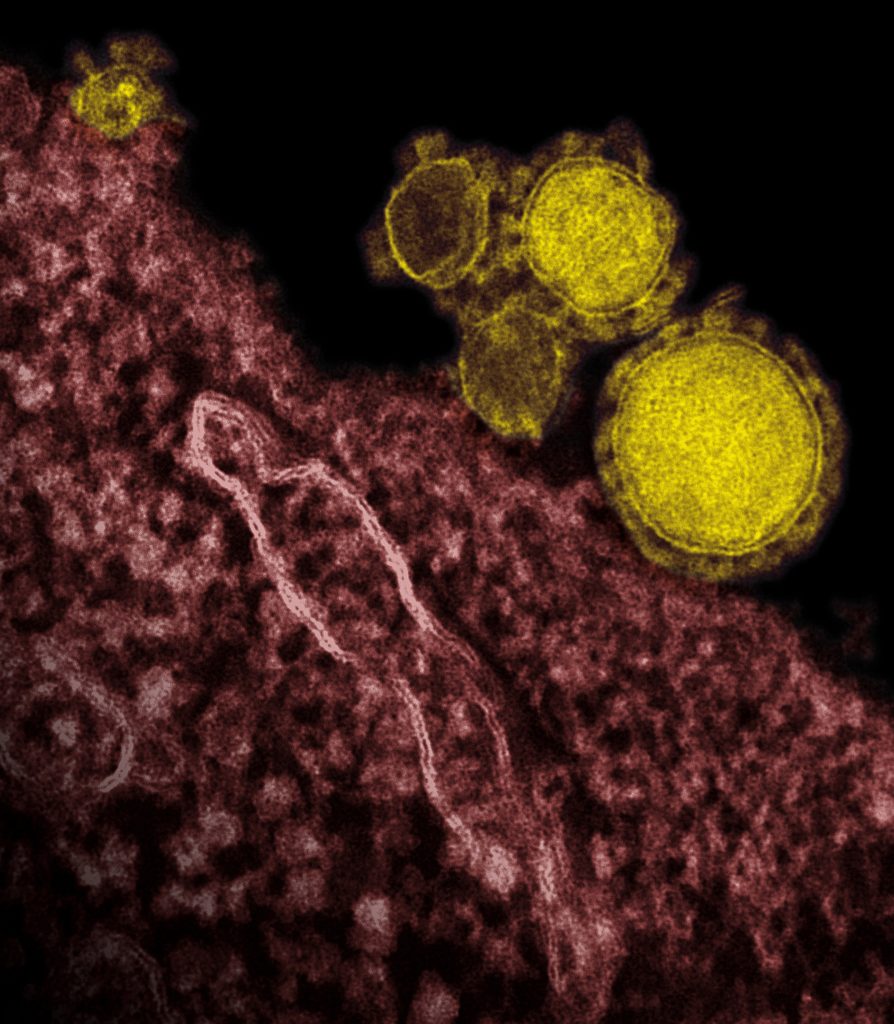
However, there may be more cases than recognised because infected camels can be identified in many parts of East and West Africa. Unlike SARS-CoV, it has not evolved to a large extent as it spreads from human to human. Thus, an outstanding question is why MERS was not recognised until 2012, or did it in fact occur, but was not diagnosed?
Both viruses cause a severe respiratory disease in humans with a high mortality. In both cases, the virus seems to evade the human immune response, resulting in an inappropriate host response to the virus, which is a major contributory factor to severe disease. A big difference between the two infections is that the severity of SARS was age-dependent, so young people (under 24 years) all survived, while those over 60 suffered a 50-percent mortality. In contrast, MERS, while also more common in older individuals, preferentially causes disease in those with underlying conditions, such as diabetes, renal failure or an immunocompromised state.
In the end, there are no vaccines or specific treatments available for either infection.
For more stunning stories and photographs from this issue, check out Asian Geographic Issue 110.